A nation’s health is the ultimate measure of its strength, serving as the bedrock upon which economic stability and social progress are built. When a government prioritizes health, it is not just funding clinics, it is investing in the productivity of its workforce and the future of its citizens.
By allocating significant resources to the healthcare sector, a country ensures that its citizens remain resilient against disease, reducing the massive economic burden that comes with untreated illnesses and sudden medical emergencies.
The governing National Democratic Congress (NDC) made a major promise in its 2024 campaign manifesto with a specific promise to remove the weight of medical bills from the shoulders of ordinary citizens.
With this vision, rooted in the belief that healthcare is a fundamental right, the NDC pledged to establish a system where no Ghanaian would be pushed into poverty simply because they fell ill. “We will implement FREE PRIMARY HEALTHCARE from the CHPS compound to the polyclinic level in the short to medium term,” the manifesto partly read.
This manifesto pledge recently materialized with the introduction of government’s Free Primary HealthCare (FPHC) policy.
What is Primary HealthCare (PHC)?
The World Health Organization describes primary healthcare as a whole-of-society approach designed to bring wellbeing closer to where people live and work. According to the WHO, this approach relies on three essential pillars:
- integrated health services to meet people’s health needs throughout their lives
- addressing the broader determinants of health through multisectoral policy and action
- empowering individuals, families and communities to take charge of their own health.
FPHC launched
On Wednesday, April 15, 2026, President John Dramani Mahama launched the Free Primary Healthcare Policy, at the Shai-Osudoku District Hospital in Accra with the aim to make primary healthcare free and accessible to citizens.
Delivering his address at the launch, he stated that primary healthcare services under the initiative will be provided at no cost to patients at the community level, adding that the policy is a complement to the National Health Insurance Scheme (NHIS) not a replacement.
“The Free Primary Healthcare complements the National Health Insurance, and so at that level it is free of charge. You go, the screening and everything is free of charge. If it is a basic illness like malaria, your CHPS compound will have the medication for malaria.
“If it is a basic illness like cholera, your CHPS compound will have the basic drugs for you. So the Free Primary Healthcare is complementary to the National Health Insurance. It is not coming to replace it, it is coming to complement it,” he said.
Nana Kofi Quakyi, a medic and country director for Aurum Institute Ghana explained the importance of the policy stating: “The logic of this policy is really rather than expecting some people to find the money, give them the money so they can do the outreach.
“It flips around the whole incentive structure from the CHPS workers waiting at the facility, which they were doing because only the services they provide there were paid for, to going out to the communities. This correction to the incentive structure benefits the most marginalized people in Ghana, which has a big equity advantage in terms of access to care,” he said.
Key points about the Free Primary Healthcare Policy?
The policy is a government initiative designed to ensure that every Ghanaian can access a defined package of essential healthcare services free of charge at the primary level. The goal is to move Ghana from “sick care” (treating illness) to “healthcare” (preventing illness).
Core Objectives
Universal Health Coverage: Aiming to increase Ghana’s coverage index from 56% to 80% by 2030.
Removing Financial Barriers: Eliminating out-of-pocket payments, which currently account for roughly 1/3 of total health expenditure.
Early Detection: Tackling the burden of disease (infectious diseases and rising non-communicable diseases like hypertension and diabetes) before they become expensive, complex emergencies.
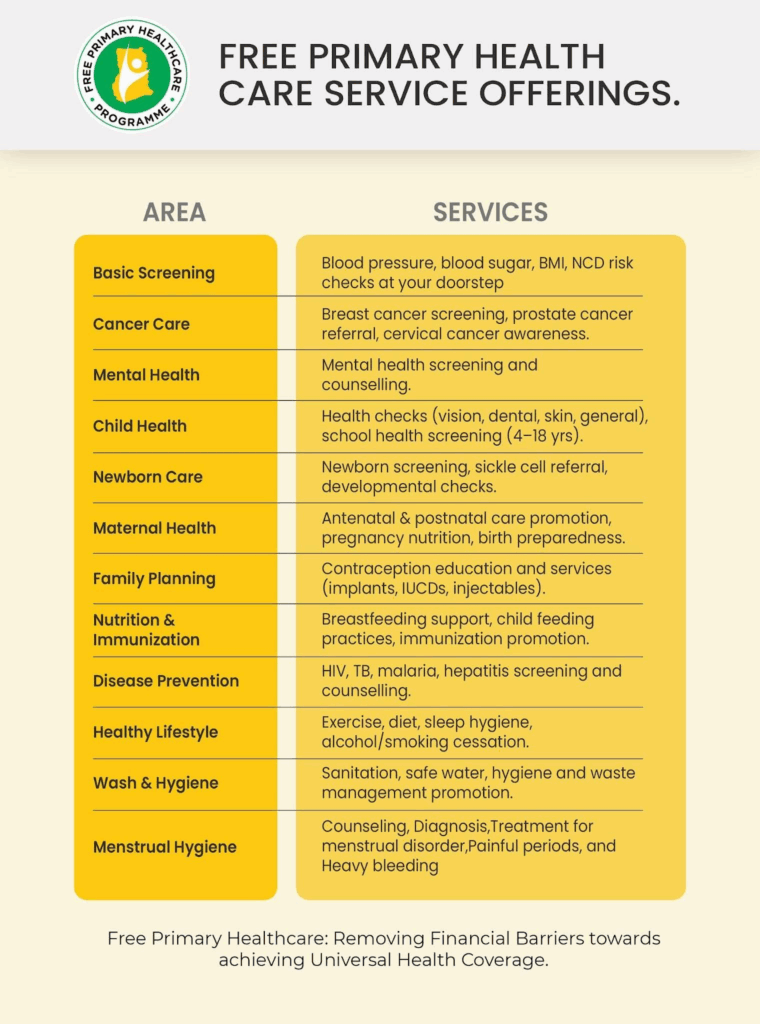
Available services under FPHC
A number of services are available under PHC, spanning routine screening, maternal and child health, treatment for common conditions, health promotion and emergency care among others.
| Category | Services Included |
| Routine Screening | Hypertension, Diabetes, Obesity, Mental Health, and Cancers. |
| Maternal & Child Health | Antenatal care, postnatal care, immunisations, and growth monitoring. |
| Common Conditions | Treatment for malaria, diarrhoea, and respiratory infections |
| Health Promotion | Risk counselling, family planning, safe water management, and menstrual hygiene. |
| Emergency Care | Basic emergency care and referral services. |
| Source: Ministry of Health | |
Where can you access FPHC
The policy is strictly applied at the Primary Healthcare Level. You can access these services at:
- CHPS Compounds
- Health Centers
- Polyclinics
- Community Outreach: Health workers will also visit homes, schools, markets (via 350+ container-based points), and workplaces.
It is important to note that for referrals to District, Regional, or Teaching hospitals, you will still need a valid National Health Insurance Scheme (NHIS) card.
Health Minister shares other logistical details
The Minister of Health, Kwabena Mintah Akandoh, announced the rollout of the Free Primary Health Care programme on Monday, April 13, 2026, during the Government Accountability Series press briefing, indicating that the Free Primary Health Care programme is designed to bring essential health services closer to communities, reducing the need for patients to travel to health facilities before accessing basic care.
“A health worker may even visit them at home,” Mr Akandoh said, adding that trained volunteers and community health workers would conduct structured screening exercises in schools, churches, workplaces and farms.
He further revealed that more than 350 container-based clinics would be deployed to high-traffic locations, including markets and lorry parks across the country.
“We will deploy trained volunteers to support our community health workforce. We will establish over 350 container-based service delivery points in high traffic areas such as, I mean, markets and lorry parks,” he said.

Reactions to FPHC rollout
The Director-General of the WHO, Dr. Tedros Adhanom Ghebreyesus, in a post on X on Thursday, April 16, commended the initiative and its potential impact on population health, stating that strong primary healthcare systems remain central to disease prevention and early treatment.
He described the policy as a significant step toward strengthening healthcare delivery and advancing Universal Health Coverage.
“This important milestone brings Ghana closer to achieving Universal Health Coverage. Strong primary health care is essential to improving population health, enabling earlier detection, timely treatment, and more effective disease prevention,” he said.
Difference between FPHC and NHIS
Speaking on Metro TV’s Good Morning Ghana on Friday April 17, 2026 former health minister, Dr. Bernard Oko Boye commended the government for prioritizing the health sector and, specifically, for throwing light on the critical areas of disease prevention and health promotion. He noted that as health advocates, it is heartening to see the ‘first gentleman’ give personal attention to these issues, as political focus often translates into much-needed financing and public awareness.
However, he balanced this praise with a critique regarding the policy’s substance, arguing that while it is presented as a new initiative, it is largely a rebranding of the existing National Health Insurance Scheme (NHIS).
He pointed out that both the registered insurance holder and the Ghana Card holder are ultimately funded by the same National Health Insurance Authority budget, with the primary difference being whether the patient paid a small registration premium or is accessing the same NHIS-funded care via a different budget line.
“When you go to our budgets, the formula, I say our because I see myself still as a friend of NHS, the money for paying the NHIS guys malaria would have been at a claims payment line… whereas the one who came with Ghana card, it will be at the level where they’ve free primary healthcare because there’s 1.2 billion in the line…
“The good thing which I will give them credit is, is that the guy who is not in the system, would have avoided the clinic… because he will say I don’t have a card. Another difference is that both don’t pay. All are paid by NHIS, but remember the guy on the system paid some 20 cedis premium when he was registered, which this guy has not paid,” he said.

Aurum Institute country lead shares more perspectives
Nana Kofi Quakyi, the Country Director for Aurum Institute Ghana, in an interview with GhanaFact provided a technical perspective on the structural necessity of the policy. He explained that while Ghana has long relied on the CHPS model for rural health, the system had suffered a “major atrophy” because the outreach components (promotion, prevention, and rehabilitation) were never actually funded.
Quakyi noted that the existing NHIS effectively only paid for “curative” services when patients showed up sick, leaving health workers with no incentive or resources to visit homes or conduct community screenings.
“By providing a structured financing mechanism specifically for these frontline services, the policy finally bridges the gap in Ghana’s health equity, ensuring that the most marginalized citizens receive care at their doorstep without the burden of transportation or opportunity costs.
To ensure the long-term sustainability of the initiative, Quakyi emphasized that the policy’s survival depends on robust data systems and a seamless patient experience. He explained that high-quality data is essential on two levels: first, to demonstrate “value for money” and health impact to the public, and second, to provide a mechanism for accountability so the government can track whether outreach is actually happening.
He warned that public confidence would only be sustained if the transition between free community-level care and the NHIS for hospital-level treatment is entirely seamless, creating a “continuum of care” that is legally protected and politically indispensable.
“The main thing with success of any public health policy and implementation is always your data… we need that performance measurement data to be able to know that, are we getting value for the money that we are spending? If we are not able to make it so that people experience a seamless transition between free primary care, NHIS, and Ghana Medical Trust Fund coverage, then public confidence is compromised.
“But as long as the funds are preserved as it is by the NHIL Act, and we’re able to make sure that the data systems are there for us to monitor and show value, then the basic political case for the policy continuing is established,” he said.
Written by Samuel Nii Adjetey


















