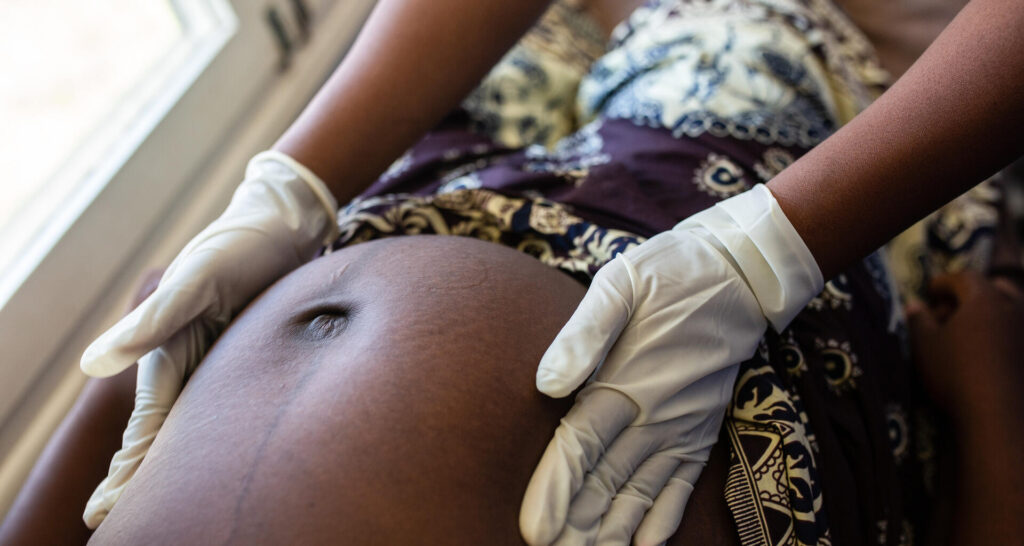
Two million women in low-resource communities have an obstetric fistula (OBF) – a neglected public health issue that results in leaking urine and/or faeces – and 100,000 more develop one every year, according to the United Nations.
The International Day to end obstetric fistula is observed every year on 23 May to ensure access to emergency obstetric care and skilled health professionals—especially midwives—to all women.
Under the theme, “End Fistula Now”, UNFPA is leading the campaign in more than 55 countries on prevention, treatment and rehabilitation efforts.
Meanwhile, in Ghana, the magnitude of the OBF is unknown, according to UNFPA Ghana.
What is an Obstetric fistula?
An obstetric fistula is a hole between the woman’s birth canal and bladder or rectum resulting from prolonged labour without medical help, leading to an uncontrollable leaking of urine, faeces, or even both.
In 2018, the international community called for obstetric fistula to be eliminated within a decade, aligning with the 2030 Agenda for Sustainable Development and its 17 global goals.
Causes
- The primary cause of obstetric fistula is difficulty in labour, where the baby’s head cannot pass through the birth canal.
- Prolonged obstructed (difficulty) in labour without access to timely high-quality medical treatment
- Lack of access to skilled birth attendants or emergency obstetric care
Symptoms
Knowing that one is suffering from Obstetric fistula often comes with the following symptoms.
- Continuous urinary incontinence with the leakage of urine uncontrollably
- Fecal incontinence with the involuntary passage of stool
- Vaginal and perineal infections due to constant exposure to urine or faeces
- An unpleasant odour arising from the constant leakage
“To end fistula, we need to make sure that all women and girls have timely access to trained midwives and high-quality obstetric care,” the UNFPA Executive Director, Dr Natalia Kanem, said.
Prevention
Prevention of Obstetric fistula is divided into three categories: Primary, Secondary, and Tertiary prevention.
- Primary prevention (social measures)
- Health promotion (programmes, policies)
- Planned pregnancies
- Birth spacing
- Contraception
- Community awareness
- Secondary prevention (Basic Obstetric Care)
- Antenatal care
- Skilled health personnel at birth
- Use of partograph
- Identification of signs and symptoms of obstructed labour
- Immediate referral
- Bladder care and/or catheterization during labour, if needed
- Tertiary prevention (more advanced Obstetric Care)
- Access to emergency obstetric and neonatal care by providing a timely, safe, quality Caesarean section by a trained/competent surgeon
- Use of an indwelling catheter to close small fresh fistulae
Treatment
The primary curative treatment remains corrective surgery; however, due to a global shortage of fistula surgeons, current treatment rates indicate that only one woman in 50 receives a fistula repair.
Obstetric fistula can often be surgically repaired through a procedure called fistula repair. Since 2003, the UNFPA has assisted with more than 121,000 significant repairs.
By: Julius Kofi Satsi